This is an excerpt from my book
Ensuring Prostate Health—No Link Found Between Androgen Levels and Risk for Prostate Cancer
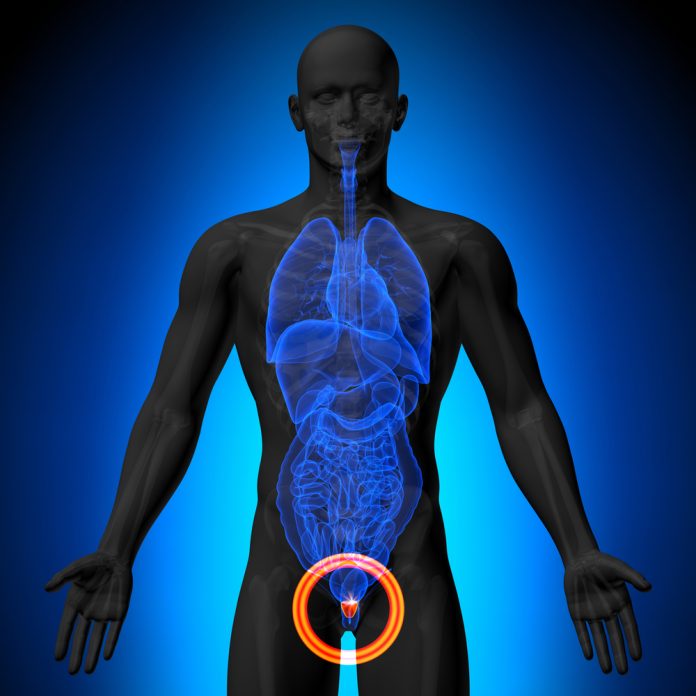
The prostate is a gland that is part of the male reproductive system. Its function is to store and secrete a slightly alkaline (pH 7.29) a milky fluid which usually constitutes 25-30% of the volume of the semen along with spermatozoa. This alkaline fluid seems to neutralize the acidity in the vagina, prolonging the lifespan of the sperm. Also, the prostate contains some?smooth muscles?that help expel semen during?ejaculation. It also helps control the flow of urine during ejaculation.
A healthy human prostate is classically said to be slightly larger than a walnut. In actuality, it is approximately the size of a kiwi fruit. It surrounds the?urethra?just below the urinary bladder and can be felt during a rectal exam.
Prostate cancer
This little gland attracts a great deal of attention in men’s health. One of the major issues is related to cancer. Prostate cancer is one of the leading causes of death in men in the United States. As men age, small hidden prostatic lesions become increasingly common. These may or may not become cancerous. These lesions occur in 30 percent of American men over the age of 45, with the prevalence rising to more than 80 percent for men over the age of 80. Genetic factors and lifestyle conditions such as diet are believed to contribute to this transformation.[Figure : The prostate and surrounding organs]
Doctors use different methods to detect prostate cancer, including prostate-specific antigen (PSA) assays, digital rectal examination (DRE), and transrectal ultrasound. A DRE before starting testosterone replacement therapy and every six months is recommended, especially for men with a family history of prostate cancer or those older than 40 years. Nobody likes having a DRE but your continued good health is worth a few seconds of discomfort. An abnormal rectal exam, a confirmed increase in PSA greater than 2 ng/mL, or PSA of over 4 ng/mL will prompt a health care provider to refer you to a urologist for further evaluation (usually an ultrasound and prostate biopsies).
Admittedly, the PSA and the DRE lack sensitivity and specificity. 25 percent of patients with prostate cancer have normal PSA levels (false negatives), while benign prostatic hyperplasia (BPH), a non-cancerous inflammation, may elevate them (false positives). Researchers have found hidden prostatic lesions with needle biopsies in some men with normal PSA level and normal transrectal ultrasound findings. Prostate biopsies are part of routine clinical use of testosterone therapy and are not justified unless a sharp rise in PSA is observed and infections have been ruled out.
There has some been confusion regarding testosterone replacement therapy’s role in PSA elevation or causing prostate cancer. Prostate cancer is initially androgen-dependent so testosterone therapy should not be used by men with prostatic cancer. This does not mean that it causes cancer. A huge pooled analysis of data from 18 studies (consisting of 3,886 men with prostate cancer and 6,438 controls), published in the February 6, 2008 issue of theJournal of the National Cancer Institute found that blood levels of androgens and other sex hormones do not seem to be related to an increased risk for prostate cancer. In short, testosterone therapy does not appear to cause prostate cancer but it can make it worse.
Prostate infection
Another health concern is prostatitis or prostate infection. This is common in aging men and can be a leading cause of an elevated PSA. Your doctor will want to check you for an infection if your PSA unexpectedly increases by checking your urine for white blood cells. If they are high, he may refer you to an urologist who would induce a discharge from your penis to look at it under the microscope. Don’t ask me how the urologist does it, ask the urologist!
Benign prostatic hyperplasia.A common health condition is benign prostatic hyperplasia or BPH. It is estimated to occur in 50 percent of men older than 50 years. Increased frequency of urination, frequent trips to the bathroom at night, incomplete voiding, and urgency to urinate indicate possible prostatic inflammation. BPH does not necessarily lead to increased rates of prostate cancer. There have been no prospective, controlled, long-term studies on the effects of testosterone administration on either the development or the progression of BPH. One open label, one-year study that measured prostate size using ultrasound found no increase during testosterone replacement therapy, suggesting that the treatment does not cause BPH. Whether testosterone treatment worsens asymptomatic BPH has not been established. Some individuals are more prone to prostatic inflammation when using testosterone.
Another study was conducted by Dr. Michael D. Trifiro at Moores UCSD Cancer Center in San Diego. Dr. Trifiro observed 158 men for 20 years to determine the correlation between serum sex hormones and lower urinary tract symptoms (reduced urinary flow, urgency, and other symptoms associated with BPH). The researchers found no significant associations of total testosterone, estradiol (E2)), testosterone: E2 ratio, DHT, or dehydroepiandrosterone with lower urinary track symptoms or with any measured hormones(published in BJU International in December 2009).
Testosterone replacement therapy is not contraindicated in those with BPH. Men with BPH who need to start testosterone replacement should be observed very closely. The first symptom that worsens with increased BPH is restricted urinary flow and urgency, especially during sleep hours. Many urologists are successfully prescribing medications to ease those symptoms and improve urinary flow in men with BPH. Finasteride (brand name:Proscar), which was approved by the FDA in 1992, inhibits production of dihydrotestosterone (DHT), which is involved with prostate enlargement. Its use can actually shrink the prostate in some men. However, many men using Proscar complain of erectile dysfunction (DHT receptors may be involved in healthy erections). For men who experience this side effect, other medications may be of help. Proscar has also been found to decrease the risk of prostate cancer in men by 25 percent over a seven year period. More studies are ongoing.
The FDA approved the drugs terazosin (brand name: Hytrin) in 1993, doxazosin (Cardura) in 1995, and tamsulosin (Flomax) in 1997 for the treatment of BPH. All three belong to the class of drugs known as alpha blockers. They work by relaxing the smooth muscle of the prostate and bladder neck to improve urine flow and to reduce bladder outlet obstruction.
Terazosin and doxazosin were developed first to treat high blood pressure. Tamsulosin is the first alpha-blocker developed specifically to treat BPH. The main side effects of these drugs are nasal congestion, lowered blood pressure, and rash or itching. Most men using them report fast improvements in their urine flow within one to three days. They end up not having to get up in the middle of the night to urinate, so they sleep better and feel less fatigued during the day.
The most common nonprescription agent used to alleviate symptoms of BPH is the over-the-counter herb saw palmetto (Serenoa repens). Extracted from the berry of the saw palmetto shrub, this substance is thought to inhibit 5-alpha reductase (5-·R), thus blocking the conversion of testosterone into DHT, which is responsible for stimulating growth of the prostate gland.
Saw palmetto is generally well tolerated; side effects are infrequent, but include headache and gastrointestinal upset. No known drug interactions are associated with the use of this herb. Some studies found that saw palmetto led to an increase in urine flow rate in men with BPH compared with placebo, with effects comparable to finasteride.
One randomized, double-blind, placebo-controlled study followed men with BPH who took standardized saw palmetto extract 160 mg or placebo twice daily for one year. There was no significant difference found between the saw palmetto and placebo groups in standardized objective urinary symptoms. The incidence of side effects was similar in the two groups. These results cast considerable doubt on the effectiveness of saw palmetto for the treatment of BPH.
Patients who cannot tolerate BPH medications are now using emerging techniques like lasers to vaporize obstructing prostate tissue (www.greenlighthps.com). Talk to your urologist about this if you’re interested. Be careful with its main side effect: you stop ejaculating forward (retrograde ejaculation into your bladder).
PERSONAL COMMENT: After using testosterone for 17 years, I started to develop a weak urine flow. My doctor gave me prescriptions for several alpha blockers (Uroxatral, Flomax, etc). They worked great but I experienced a rash with each one. My urologist found a prostate infection, which he treated with antibiotics. The infection seemed to linger for months. I then received an ultrasound of my prostate. This test showed that my prostate was not enlarged. Instead it showed that a calcification, caused by a chronic prostatic infection, was blocking my urine flow through my prostate. I got the green light laser procedure done to open up my urethra. It worked great. So, what may seem like BPH may not be! Prostatic infections often go untreated for months since in many cases we may not have symptoms.
Prostate Ultrasound Test
CLICK HERE TO BUY AN AFFORDABLE TESTOSTERONE TEST- NO DOCTOR VISIT
Here are more studies about testosterone and prostate cancer:
https://www.excelmale.com/threads/431…Michael-Scally
https://www.excelmale.com/threads/143…cer-Found-Safe
https://www.excelmale.com/threads/439…rostate-Cancer
VIDEO: Does testosterone cause prostate cancer? Interview with Dr. Justin Saya from Defy Medical
Recent Posts
Sleep is Anabolic- By Dr Mauro Di Pasquale
SLEEP IS ANABOLIC
Dr. Mauro Di Pasquale, M.D.
There are a lot of factors that impact on body composition including the two that are uppermost in...
What is a Normal Blood Level of Testosterone?
Normal values may vary from lab to lab depending on what reference range they use. Your doctor will have your test results in one...
Testosterone Experts Debunk Common Myths
Dr. Abraham Morgentaler, an Associate Clinical Professor at Harvard Medical School and Beth Israel Deaconess Medical Center in Boston, MA, gives an overview of...
Dr. Eugene Shippen Lectures About HRT in Women
Dr. Eugene Shippen is one of the most respected physicians in hormone replacement for men and women. Here he is lecturing to physicians at one...
How to Inject Testosterone Safely
In this video the folks from Defy Medical show how to safely inject testosterone in the glutes.
The following information was taken from the book:...