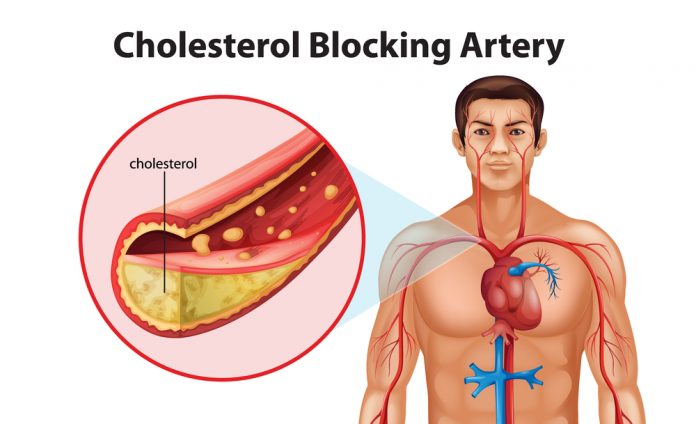
Higher dose testosterone can decrease HDL.
Click here for background information:
Why does testosterone therapy decrease HDL cholesterol in some men?HDL (High Density Lipoprotein cholesterol) particles are sometimes referred to as “good cholesterol” because they can transport fat molecules out of artery walls, reduce macrophage accumulation, and thus help prevent or even regress atherosclerosis.
Data from the landmark Framingham Heart Study showed that, for a given level of LDL, the risk of heart disease increases 10-fold as the HDL varies from high to low. On the converse, however, for a fixed level of HDL, the risk increases 3-fold as LDL varies from low to high.
While higher HDL levels are correlated with cardiovascular health, no medication used to increase HDL has been proven to improve health.In other words, while high HDL levels might correlate with better cardiovascular health, specifically increasing one’s HDL might not increase cardiovascular health. The remaining possibilities are that either good cardiovascular health causes high HDL levels, there is some third factor which causes both, or this is a coincidence with no causal link.
Pharmacologic (1- to 3-gram/day) niacin doses increase HDL levels by 10–30%,making it the most powerful agent to increase HDL-cholesterol. A randomized clinical trial demonstrated that treatment with niacin can significantly reduce atherosclerosis progression and cardiovascular events.However, niacin products sold as “no-flush”, i.e. not having side-effects such as “niacin flush”, do not contain free nicotinic acid and are therefore ineffective at raising HDL, while products sold as “sustained-release” may contain free nicotinic acid, but “some brands are hepatotoxic”; therefore the recommended form of niacin for raising HDL is the cheapest, immediate-release preparation.[Both fibrates and niacin increase artery toxic homocysteine , an effect that can be counteracted by also consuming a multivitamin with relatively high amounts of the B-vitamins, however multiple European trials of the most popular B-vitamin formulas, trial showing 30% average reduction in homocysteine, while not showing problems have also not shown any benefit in reducing cardiovascular event rates. A 2011 niacin study was halted early because patients adding niacin to their statin treatment showed no increase in heart health, but did experience an increase in the risk of stroke.
Plasma HDL Cholesterol as a Noncausal Biomarker
Abbreviations:
SNPs: A single-nucleotide polymorphism, is a variation (mutation) in a single nucleotide that occurs at a specific position in the genome, where each variation is present to some appreciable degree within a population.
CHD: Coronary Heart Disease
HDL: High Density Lipoprotein
MI: Myocardial infarction
Pleiotropic effects: occur when one gene influences two or more seemingly unrelated phenotypic traits. Therefore, a mutation in a pleiotropic gene may have an effect on several traits simultaneously due to the gene coding for a product used by a myriad of cells or different targets that have the same signaling function.There is a strong inverse association of plasma HDL-C concentrations with CHD, which for decades lent credence to the notion that pharmacological raising of HDL-C should protect against CHD. Yet recent genetic analyses have in general failed to support a causal role for HDL-C in CHD. As related above, a genetic score comprising LDL-C–associated SNPs was found to have a strong relationship with MI risk. The same study performed a parallel Mendelian randomization study in >50 000 cases and controls using a genetic score comprising 14 GWAS SNPs primarily associated with plasma HDL-C levels. Whereas a 1-standard deviation increase in HDL-C (≈15 mg/dL) was expected to be associated with a 38% decrease in MI risk using data from observational epidemiological studies, a 1- standard deviation decrease in HDL-C because of genetic score conferred no significant change in MI risk .
The same study performed a more focused Mendelian randomization analysis on a coding SNP (Asn396Ser) in the LIPG gene, which encodes endothelial lipase, an enzyme that metabolizes HDL particles but has little effect on plasma LDL-C and triglycerides. To obtain adequate power for the analysis, the SNP was genotyped in ≈20 000 individuals with MI and 95 000 control individuals. Carriers of the LIPG Asn396Ser SNP variant had increased plasma HDL-C levels, on average ≈5.5 mg/dL. This degree of increase in HDL-C was expected to be associated with a 13% decrease in MI risk using data from observational epidemiological studies. However, carriers of the LIPG Asn396Ser variant were found to have a negligible change in MI risk (1% decrease; P=0.85; 95% confidence interval ranging from an 11% increase to a 12% decrease), essentially ruling out an effect of LIPG on the pathogenesis of CHD. In other studies, genetic analyses of both common variants in the ABCA1 gene, which encodes the ATP-binding-cassette transporter A1 involved in reverse cholesterol transport, and rare variants in the same gene that are linked to familial hypoalphalipoproteinemia and Tangier disease and have been unable to demonstrate a relationship between decreased plasma HDL-C levels in affected individuals and increased CHD risk.
In contrast to LDL-C, the collective genetic data suggest that HDL-C is not causal for CHD risk, at least in a simplistic sense. Although the data cannot rule out that there are some biological mechanisms that lead to increased plasma HDL-C levels that also protect against CHD, it seems fair to conclude that not all interventions that raise HDL-C will reduce CHD risk. Further support for this conclusion is provided by RCT (randomized controlled) data, most notably with the cholesteryl ester transfer protein (CETP) inhibitors, which substantially raise plasma HDL-C levels. Three inhibitors of CETP—torcetrapib, dalcetrapib, and evacetrapib—all raised HDL- C substantially, and each failed to reduce risk for CHD in large-scale RCTs. All 3 studies— the Investigation of Lipid Level Management to Understand Its Impact in Atherosclerotic Events (ILLUMINATE) trial of torcetrapib, which increased HDL-C by 70%; the dal- OUTCOMES trial of dalcetrapib, which increased HDL-C by 30%; and the Assessment of Clinical Effects of Cholesteryl Ester Transfer Protein Inhibition With Evacetrapib in Patients at a High-Risk for Vascular Outcomes (ACCELERATE) trial of evacetrapib, which was projected to raise HDL-C by > 90%—were all terminated prematurely because of lack of clinical efficacy. Indeed, torcetrapib seemed to result in increased cardiovascular events and death, although this has been attributed to off-target, nonlipid-related effects of this particular medication.Source: Circ Res. 2016 Feb 19;118(4):579-85.
The CANHEART study showed that HDL lower than 30 mg/dL increase risk of death caused by cardiovascular disease and cancer. The higher HDL levels over 70 did not seem as protective as 40-70.
Source

For more discussions on HDL and TRT, click on this link: