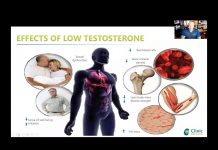
Who is a Candidate for Testosterone Replacement Therapy?
By Abraham Morgentaler, M.D.
There is consensus that candidates for treatment with Testosterone Replacement Therapy should have signs or symptoms of TESTOSTERONE DEFICIENCY combined with biochemical evidence of low T levels.13 The challenge, however, is deciding what T level is considered low. For the first 40 years after the commercial availability of T products, the diagnosis was made entirely on clinical presentation. With the introduction of readily available testing with the development of radioimmunoassays in the 1970s, the emphasis shifted to documentation of low blood levels. Today, it is becoming increasingly clear that symptoms and clinical presentation should once again take priority,13 with blood test results an important, yet secondary confirmation.
The difficulty with arriving at a reasonable threshold value for biochemical confirmation of TESTOSTERONE DEFICIENCYis underscored by the wide range of recommended thresholds offered by various professional groups and experts, ranging from 200 ng/dl (approximately 7 nmol/l) to 400 ng/dl (approximately 14 nmol/l).13 This confusing situation is worsened by the recommendation by the Endocrine Society in 2010 to follow reference ranges provided by the laboratory performing the testosterone testing,14 because there is so much variation in reference ranges across laboratories that one survey revealed that 17 of 25 laboratories had different reference ranges.15 This means that the same test result may be categorized as normal by one laboratory and low by another.
The explanation for the wide range in threshold recommendations is that there is no specific T value that reliably separates men who may benefit from treatment from those who will not.14Threshold recommendations are therefore arbitrary. The application of lower thresholds means that a higher rate of treated men are likely to experience benefits, but at the cost of denying treatment to many men who may also benefit. Higher thresholds allow for inclusion of more candidates who may benefit, yet overall response rates may be lower.16 Moreover, there is a substantial degree of inter-individual variability with regard to symptoms and response to treatment, due at least, in part, to two known confounders—the binding of androgen to sex hormone binding globulin and genetic variability with regard to the number of CAG repeats in the androgen receptor gene, with larger numbers of repeats associated with reduced sensitivity.17 This means that healthcare providers must decide on whether a course of treatment is indicated based on the totality of clinical presentation rather than by a blood test result alone.
In our practice, we have found free testosterone to be more clinically useful than total testosterone, as it is independent of sex hormone binding globulin variability.18 Values <1.5 ng/dl for direct free T measurement or <100 pg/ml for calculated free T are consistent with a diagnosis of TESTOSTERONE DEFICIENCY in symptomatic men.16 and 19We routinely measure both total and free testosterone during the evaluation and also to monitor response to treatment.
The current widespread practice by health insurance companies, including Medicare, to restrict coverage based on specific testosterone threshold values therefore lacks a scientific basis and is contrary to good medical practice. The diagnosis of TESTOSTERONE DEFICIENCY requires clinical judgment, and attempts to replace this with irrational adherence to arbitrarily selected values prevent healthcare providers from offering important treatments to appropriately selected patients.