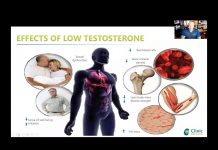
Benefits associated with lowered serum DHT levels after 5α-reductase inhibitor (5AR-I) therapy in men have contributed to a misconception that circulating DHT levels are an important stimulus for androgenic action in target tissues (e.g., prostate). Yet evidence from clinical studies indicates that intracellular concentrations of androgens (particularly in androgen-sensitive tissues) are essentially independent of circulating levels.
To assess the clinical significance of modest elevations in serum DHT and the DHT/testosterone (T) ratio observed in response to common T replacement therapy, a comprehensive review of the published literature was performed to identify relevant data. Although the primary focus of this review is about DHT in men, we also provide a brief overview of DHT in women. The available published data are limited by the lack of large, well-controlled studies of long duration that are sufficiently powered to expose subtle safety signals. Nonetheless, the preponderance of available clinical data indicates that modest elevations in circulating levels of DHT in response to androgen therapy should not be of concern in clinical practice. Elevated DHT has not been associated with increased risk of prostate disease (e.g., cancer or benign hyperplasia) nor does it appear to have any systemic effects on cardiovascular disease safety parameters (including increased risk of polycythemia) beyond those commonly observed with available T preparations. Well-controlled, long-term studies of transdermal DHT preparations have failed to identify safety signals unique to markedly elevated circulating DHT concentrations or signals materially different from T.
Essential Points:
- Circulating levels of DHT in response to testosterone replacement therapy (TRT) do not correlate with those found in androgen sensitive tissue (e.g., prostate, adipose, muscle) due to local regulatory mechanisms that tightly control intracellular androgen homeostasis.
- The modest increases observed in serum DHT and in the DHT/T ratio observed after TRT are unlikely to be a cause of clinical concern, particularly when viewed in the context of changes observed in these parameters for currently marketed T-replacement products and those under development for which DHT data are available.
- While well-controlled, long-term studies designed to specifically examine the effects of androgen exposure on risk for prostate need to be conducted, the current clinical data base is relatively reassuring that circulating levels of androgens (or changes in such) apparently do not play as pivotal a role as once thought in the development of prostate disease.
- Robust epidemiologic or clinical trial evidence of a deleterious DHT effect on CVD is lacking. There is some evidence that DHT therapy in men with CVD may improve clinical status—a finding that needs confirmation. Data from a longitudinal data base of older normal (i.e., not hypogonadal) indicated an association between serum DHT and incident CV disease and mortality. Conversely, others have reported that higher DHT levels in older men were associated with decreased all-cause mortality and reduced ischemic heart disease mortality. Additional exploration in prospective, placebo-controlled intervention studies of TRT with CVD as the primary endpoint is needed to resolve the long-term effects of androgens on CVD risks.
- DHT does not play a substantive role in body composition compared to T under normal conditions. Thus, elevated levels of DHT in response to TRT are unlikely to appreciably impact lean or fat mass. Nonetheless, data from animals suggest a role for DHT in adipose tissue that inhibits biochemical pathways involved in lipid synthesis and promotes several transcripts associated with apoptosis of adipocytes. Whether these DHT-induced effects also occur in human adipose tissue remains an area for future study.
- There is very limited data available regarding DHT and effects on cognition. Further research is needed, particularly in light of animal data where DHT positively modified synaptic structure and significantly delayed cognitive impairment in a well-regarded animal model for Alzheimer’s disease.
- Recent data indicating that higher levels of DHT were inversely associated with insulin resistance and risk of diabetes merit further mechanistic investigation to understand whether this action is separate from that of T.
- Perhaps the most controversial area with regards to the nonprostate-related effects of DHT in male health is in the area of sexual function, particularly with respect to the reversibility, or lack thereof, of sexual side effects that are attributed to the 5AR-Is. Multiple large studies have reported sexual dysfunction in men with BPH taking finasteride or dutasteride, including three large, placebo-controlled studies . Overall, use of 5AR-Is is associated with a 5% to 9% prevalence of new-onset erectile dysfunction and decreased libido . These data strongly point to a role for endogenous DHT in the maintenance of normal sexual and ejaculatory function and sexual desire. And, in fact, this has been shown to be true in healthy young men in whom serum DHT concentration was revealed to be the sole independent predictor of orgasm frequency, a surrogate for overall male sexual function.